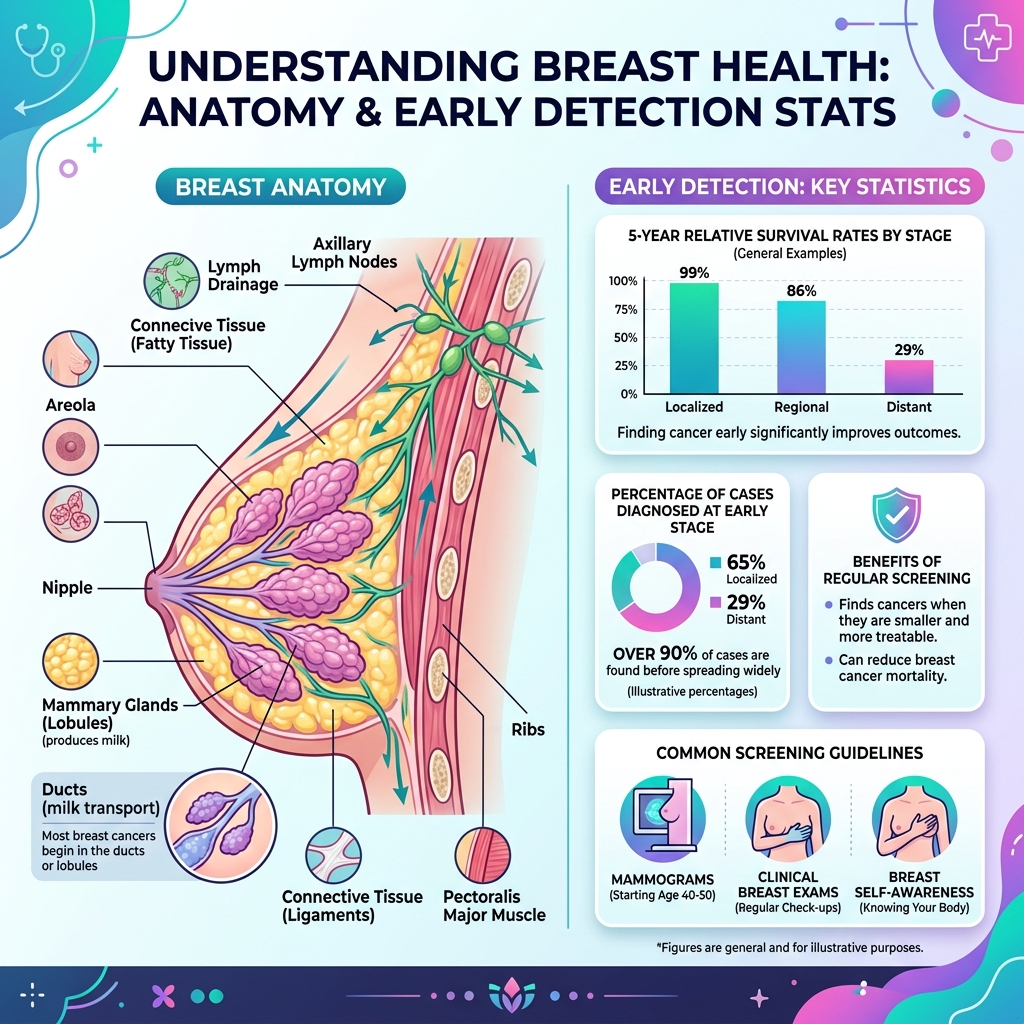
Introduction
Let’s be honest—health checkups rarely top anyone’s “fun things to do” list. But when it comes to screening for breast cancer, a simple appointment could literally save your life. Early detection gives you options, confidence, and time—three things you never want to lose.
Whether you’re scheduling your first mammogram or helping a loved one understand their risks, knowing how screening works can take away a lot of fear. Think of it like changing the batteries in a smoke alarm. It’s quick, a little inconvenient, but absolutely worth it.
What Is Screening for Breast Cancer and Why Is It Important?
Screening for breast cancer means checking for signs of cancer before symptoms appear. You might feel perfectly healthy, yet tiny changes could already be happening inside the breast tissue. Screening helps catch those changes early—sometimes years before you’d notice anything yourself.
Here’s the thing:
When detected early, breast cancer survival rates increase dramatically. Treatment is often less aggressive, recovery is quicker, and outcomes are better.
Why early detection matters
- Smaller tumors are easier to treat
- Lower treatment costs
- Less invasive procedures
- Higher survival rates
- Peace of mind
It’s not about being scared—it’s about being prepared and in control.
Common Methods Used in Screening for Breast Cancer
There isn’t just one way to check for breast cancer. Doctors use several breast cancer screening methods, depending on age, risk, and family history.
H3: Mammogram
The gold standard of screening for breast cancer.
A low-dose X-ray that can detect tiny lumps long before they’re felt. Most women over 40 are advised to get one regularly.
H3: Clinical Breast Exam
Performed by a doctor or nurse during a routine visit. They check for lumps or unusual changes.
H3: Breast Self-Exam
Not a replacement for medical screening, but helpful for awareness. Understanding what’s normal for your body makes it easier to notice changes quickly.
H3: MRI or Ultrasound
Recommended for women with higher risk factors or dense breast tissue. These tools offer deeper imaging.
Sometimes, combining methods gives the clearest picture.
When Should You Start Screening for Breast Cancer?
This is the question everyone asks. And the answer? It depends.
General recommendations
- 20s–30s: Self-awareness + clinical exams
- 40–44: Optional mammograms
- 45–54: Annual mammograms
- 55+: Every 1–2 years
H3: Breast cancer screening guidelines India
In India, experts often recommend:
- Mammograms starting at 40
- Earlier screening if family history exists
- Regular clinical exams in primary care visits
Because awareness is still growing, many women discover issues late. That’s why proactive screening for breast cancer is becoming more strongly encouraged across the country.
Screening for Breast Cancer for High-Risk Women
Some people need closer monitoring. If you fall into a higher-risk group, waiting until 40 might not be ideal.
High risk breast cancer screening guidelines include:
- Family history (mother/sister with breast cancer)
- Genetic mutations (BRCA1/BRCA2)
- Previous chest radiation
- Personal history of breast conditions
Extra precautions may involve:
- Earlier mammograms (as early as 30)
- Annual MRI + mammogram
- Genetic counseling
- More frequent checkups
If you’re unsure, talk to your doctor. Better safe than sorry, right?
📸 Suggested Image Placement:
Mid-article – Comparison table or visual of mammogram vs MRI vs ultrasound
What Happens During Screening for Breast Cancer?
If you’ve never had a mammogram, you might picture something scary. But honestly? It’s usually done in 15–20 minutes.
Here’s how it goes:
- You change into a gown
- The breast is placed between two plates
- Gentle compression for a few seconds
- X-ray images taken
Yes, it can feel slightly uncomfortable—but it’s quick. Think “momentary pressure,” not pain.
Many women say the anxiety beforehand is worse than the test itself.
Real-Life Story: A Small Appointment That Changed Everything
My friend Neha almost skipped her annual checkup. Work deadlines, kids’ schedules—you know how life piles up.
But she went anyway.
Her screening for breast cancer detected a tiny lump she couldn’t feel. Stage 1. Treatable. Surgery was minor, and she was back home within days.
She often says, “That single hour made all the difference—it saved my life.”
Stories like hers aren’t rare. They’re the reason screening matters.
Benefits and Myths About Screening for Breast Cancer
Benefits
- Early diagnosis
- Better survival rates
- Less aggressive treatment
- Emotional reassurance
Common myths busted
❌ “I feel healthy, so screening isn’t necessary.”
✔ Cancer can exist without symptoms
❌ “Mammograms cause cancer”
✔ Radiation exposure is extremely low
❌ “Only older women need it”
✔ Younger women with risks need screening too
Sometimes fear spreads faster than facts. Understanding the facts helps you make better decisions.
How to Prepare for Your Screening Appointment
A few small steps can make the experience smoother.
Tips:
- Avoid deodorant or lotions (they affect imaging)
- Wear a two-piece outfit
- Schedule after your period (less tenderness)
- Bring previous reports
And maybe reward yourself afterward. Coffee date? Movie? Make it feel less clinical and more like self-care.
Making Screening a Habit, Not a Hassle
Health routines work best when they’re automatic. Like brushing teeth.
Try:
- Setting calendar reminders
- Booking annual appointments in advance
- Pairing visits with a friend
- Tracking reports digitally
Regular screening for breast cancer becomes easier when it’s part of your yearly rhythm.
📸 Suggested Image Placement:
Before Conclusion – Smiling woman with family, CTA overlay like “Early Detection Saves Lives”
Conclusion
At the end of the day, screening for breast cancer isn’t just a medical test—it’s a gift you give yourself and your family. It’s choosing prevention over panic, awareness over uncertainty. A small step today can protect years of tomorrow. So don’t wait for symptoms or “the right time.” Book that appointment, encourage someone you love, and stay proactive. Your future self will thank you.
👉 Call to Action:
Schedule your screening today and talk to your doctor about the right plan for you. Explore our related guides on women’s wellness and preventive health for more support.
Frequently Asked Questions (FAQs)
1. How often should I go for screening for breast cancer?
Most women over 45 should have yearly or biennial mammograms. High-risk women may need annual scans.
2. Are mammograms painful?
They may feel slightly uncomfortable but only for a few seconds.
3. What are the best breast cancer screening methods?
Mammograms, clinical exams, MRIs, and ultrasounds depending on risk level.
4. What are High risk breast cancer screening guidelines?
Earlier and more frequent testing, often combining MRI and mammograms.
5. What are Breast cancer screening guidelines India?
Typically begin at 40, with earlier testing for women with risk factors.